|
The supply side of digital health tools and tech is growing at a hockey-stick pace. There are mobile apps and remote health monitors, digital therapeutics and wearable tech from head-to-toe. Today in America, electronic health records (EHRs) are implemented in most physician offices and virtually all hospitals. Chapter 5 of my book, HealthConsuming: From Health Consumer to Health Citizen, details the promise of digital health: wearable, shareable and virtual.
Broadband connectivity, cloud computing, data analytics and well-conceived artificial intelligence (AI) enable the use of data generated from digital health tools to benefit our health. Increasingly, as connectivity gets to each of us wherever we live, work, play, and learn, and sensors shrink and lower in cost, we can do more self-care at home and in lower-cost venues to help bend that stubborn medical cost curve. This is a health economist’s Holy Grail, and my vision for the home-as-health-hub which is my end-image in HealthConsuming. As I walk the miles of aisles at the annual CES, I track ten technology categories that can support this paradigm, covering more mature digital health tech like WiFi weight scales and personal emergency response systems to the growing Internet of Things ecosystem for smart and connected homes and cars, an emerging third space for health that Honda, Mercedes, Toyota, et. al., are concepting, which I wrote about back in 2007 focusing on Toyota’s wellness car concept. Promising, promising. With every one of these digital health encounters, from Alexa to Zipongo, a bit of data is created. It’s personal stuff, and it’s a tiny little bit about “you.” All that digital dust can be collected, mashed up and built into a personal profile for your benefit, or for other reasons. The graphic is based on work done by Juhan Sonin of GoInvo, a group that does brilliant work on health data design that’s vigilantly people-focused. GoInvo has been working for a long time on how to communicate health and healthcare data in enchanting ways. Juhan and another person first shaped my views converging the promise of digital health data through enchanting design, and the perils of Big Data algorithms. Juhan for the former lightbulb moment; and for the latter, Fred Trotter. I interviewed Fred for research I was conducted on behalf of the California HealthCare Foundation (CHCF) in 2014. For CHCF that year, I wrote Here’s Looking at You: How Personal Health Information is Being Tracked and Used, I took cues from a 60 Minutes‘ profile of third-party data brokers and Latanya Sweeney’s groundbreaking research at the Harvard Privacy Lab. Latanya found that just a few data points — which fell out of HIPAA-privacy protected flows — could re-identify a person with, say, HIV positive status, a mental health DSM-code, or degenerative disease. Five years later, patients still share their personal health information on Facebook groups, with the promise of crowdsourcing cures, accessing support and advice, and finding community. As a WEGO Health poll of patient activists found in April 2019, patients continue to share this very intimate data, even in the wake of the Facebook/Cambridge Analytica story, growing cybersecurity breaches of medical data, and a challenging environment for trust and “fake news” for health care. In researching the thorny privacy issues for HealthConsuming,. I learned the phrase “a concerned embrace of technology” from Deloitte’s 2017 survey of U.S. mobile consumers. Deloitte found that 80% of consumers believed that companies were using their personal data and that their data wsa being shaerd with third parties. But people were williong to share “some” online data (like name or email address), less willing to share health metrics using a phone or wearable device — only 7% of people willing to do that in 2017 based on this poll. So “concerned embrace” for health means that trust is the enabling bridge between digital health connections and peoples’ willingness to share data — underpinned by stronger privacy protections and true data ownership for each person. Through that ownership and control, people could monetize their own data and treat it as the personal asset it truly is. This is the plotline between HealthConsuming‘s Chapter 5 on the promise of “Digital Health: Wearable, Shareable, Virtual” and Chapter 6 on “Privacy and Health Data In-Security.” Tomorrow will be my fifth and final post in this week’s series outlining HeatlhConsuming: From Health Consumer to Health Citizen, focusing on the last two words in the title. Can and will Americans take on the role of health citizens, with health care access as a civil right and full privacy protections, coupled with the responsibilities for self-care and health engagement, and the civic responsibility to vote and engage in civil discourse? We’ll round out this journey in tomorrow’s Health Populi. That’s the argument for health citizenship, our topic for tomorrow’s #5 of five posts plotlining HealthConsuming: From Health Consumer to Health Citizen, all this week in the Health Populi blog. The post The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 appeared first on HealthPopuli.com. The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 posted first on http://dentistfortworth.blogspot.com via Blogger The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4
0 Comments
The supply side of digital health tools and tech is growing at a hockey-stick pace. There are mobile apps and remote health monitors, digital therapeutics and wearable tech from head-to-toe. Today in America, electronic health records (EHRs) are implemented in most physician offices and virtually all hospitals. Chapter 5 of my book, HealthConsuming: From Health Consumer to Health Citizen, details the promise of digital health: wearable, shareable and virtual.
Broadband connectivity, cloud computing, data analytics and well-conceived artificial intelligence (AI) enable the use of data generated from digital health tools to benefit our health. Increasingly, as connectivity gets to each of us wherever we live, work, play, and learn, and sensors shrink and lower in cost, we can do more self-care at home and in lower-cost venues to help bend that stubborn medical cost curve. This is a health economist’s Holy Grail, and my vision for the home-as-health-hub which is my end-image in HealthConsuming. As I walk the miles of aisles at the annual CES, I track ten technology categories that can support this paradigm, covering more mature digital health tech like WiFi weight scales and personal emergency response systems to the growing Internet of Things ecosystem for smart and connected homes and cars, an emerging third space for health that Honda, Mercedes, Toyota, et. al., are concepting, which I wrote about back in 2007 focusing on Toyota’s wellness car concept. Promising, promising. With every one of these digital health encounters, from Alexa to Zipongo, a bit of data is created. It’s personal stuff, and it’s a tiny little bit about “you.” All that digital dust can be collected, mashed up and built into a personal profile for your benefit, or for other reasons. The graphic is based on work done by Juhan Sonin of GoInvo, a group that does brilliant work on health data design that’s vigilantly people-focused. GoInvo has been working for a long time on how to communicate health and healthcare data in enchanting ways. Juhan and another person first shaped my views converging the promise of digital health data through enchanting design, and the perils of Big Data algorithms. Juhan for the former lightbulb moment; and for the latter, Fred Trotter. I interviewed Fred for research I was conducted on behalf of the California HealthCare Foundation (CHCF) in 2014. For CHCF that year, I wrote Here’s Looking at You: How Personal Health Information is Being Tracked and Used, I took cues from a 60 Minutes‘ profile of third-party data brokers and Latanya Sweeney’s groundbreaking research at the Harvard Privacy Lab. Latanya found that just a few data points — which fell out of HIPAA-privacy protected flows — could re-identify a person with, say, HIV positive status, a mental health DSM-code, or degenerative disease. Five years later, patients still share their personal health information on Facebook groups, with the promise of crowdsourcing cures, accessing support and advice, and finding community. As a WEGO Health poll of patient activists found in April 2019, patients continue to share this very intimate data, even in the wake of the Facebook/Cambridge Analytica story, growing cybersecurity breaches of medical data, and a challenging environment for trust and “fake news” for health care. In researching the thorny privacy issues for HealthConsuming,. I learned the phrase “a concerned embrace of technology” from Deloitte’s 2017 survey of U.S. mobile consumers. Deloitte found that 80% of consumers believed that companies were using their personal data and that their data wsa being shaerd with third parties. But people were williong to share “some” online data (like name or email address), less willing to share health metrics using a phone or wearable device — only 7% of people willing to do that in 2017 based on this poll. So “concerned embrace” for health means that trust is the enabling bridge between digital health connections and peoples’ willingness to share data — underpinned by stronger privacy protections and true data ownership for each person. Through that ownership and control, people could monetize their own data and treat it as the personal asset it truly is. This is the plotline between HealthConsuming‘s Chapter 5 on the promise of “Digital Health: Wearable, Shareable, Virtual” and Chapter 6 on “Privacy and Health Data In-Security.” Tomorrow will be my fifth and final post in this week’s series outlining HeatlhConsuming: From Health Consumer to Health Citizen, focusing on the last two words in the title. Can and will Americans take on the role of health citizens, with health care access as a civil right and full privacy protections, coupled with the responsibilities for self-care and health engagement, and the civic responsibility to vote and engage in civil discourse? We’ll round out this journey in tomorrow’s Health Populi. That’s the argument for health citizenship, our topic for tomorrow’s #5 of five posts plotlining HealthConsuming: From Health Consumer to Health Citizen, all this week in the Health Populi blog. The post The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 appeared first on HealthPopuli.com. The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 posted first on http://dentistfortworth.blogspot.com via Blogger The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 The supply side of digital health tools and tech is growing at a hockey-stick pace. There are mobile apps and remote health monitors, digital therapeutics and wearable tech from head-to-toe. Today in America, electronic health records (EHRs) are implemented in most physician offices and virtually all hospitals. Chapter 5 of my book, HealthConsuming: From Health Consumer to Health Citizen, details the promise of digital health: wearable, shareable and virtual.
Broadband connectivity, cloud computing, data analytics and well-conceived artificial intelligence (AI) enable the use of data generated from digital health tools to benefit our health. Increasingly, as connectivity gets to each of us wherever we live, work, play, and learn, and sensors shrink and lower in cost, we can do more self-care at home and in lower-cost venues to help bend that stubborn medical cost curve. This is a health economist’s Holy Grail, and my vision for the home-as-health-hub which is my end-image in HealthConsuming. As I walk the miles of aisles at the annual CES, I track ten technology categories that can support this paradigm, covering more mature digital health tech like WiFi weight scales and personal emergency response systems to the growing Internet of Things ecosystem for smart and connected homes and cars, an emerging third space for health that Honda, Mercedes, Toyota, et. al., are concepting, which I wrote about back in 2007 focusing on Toyota’s wellness car concept. Promising, promising. With every one of these digital health encounters, from Alexa to Zipongo, a bit of data is created. It’s personal stuff, and it’s a tiny little bit about “you.” All that digital dust can be collected, mashed up and built into a personal profile for your benefit, or for other reasons. The graphic is based on work done by Juhan Sonin of GoInvo, a group that does brilliant work on health data design that’s vigilantly people-focused. GoInvo has been working for a long time on how to communicate health and healthcare data in enchanting ways. Juhan and another person first shaped my views converging the promise of digital health data through enchanting design, and the perils of Big Data algorithms. Juhan for the former lightbulb moment; and for the latter, Fred Trotter. I interviewed Fred for research I was conducted on behalf of the California HealthCare Foundation (CHCF) in 2014. For CHCF that year, I wrote Here’s Looking at You: How Personal Health Information is Being Tracked and Used, I took cues from a 60 Minutes‘ profile of third-party data brokers and Latanya Sweeney’s groundbreaking research at the Harvard Privacy Lab. Latanya found that just a few data points — which fell out of HIPAA-privacy protected flows — could re-identify a person with, say, HIV positive status, a mental health DSM-code, or degenerative disease. Five years later, patients still share their personal health information on Facebook groups, with the promise of crowdsourcing cures, accessing support and advice, and finding community. As a WEGO Health poll of patient activists found in April 2019, patients continue to share this very intimate data, even in the wake of the Facebook/Cambridge Analytica story, growing cybersecurity breaches of medical data, and a challenging environment for trust and “fake news” for health care. In researching the thorny privacy issues for HealthConsuming,. I learned the phrase “a concerned embrace of technology” from Deloitte’s 2017 survey of U.S. mobile consumers. Deloitte found that 80% of consumers believed that companies were using their personal data and that their data wsa being shaerd with third parties. But people were williong to share “some” online data (like name or email address), less willing to share health metrics using a phone or wearable device — only 7% of people willing to do that in 2017 based on this poll. So “concerned embrace” for health means that trust is the enabling bridge between digital health connections and peoples’ willingness to share data — underpinned by stronger privacy protections and true data ownership for each person. Through that ownership and control, people could monetize their own data and treat it as the personal asset it truly is. This is the plotline between HealthConsuming‘s Chapter 5 on the promise of “Digital Health: Wearable, Shareable, Virtual” and Chapter 6 on “Privacy and Health Data In-Security.” Tomorrow will be my fifth and final post in this week’s series outlining HeatlhConsuming: From Health Consumer to Health Citizen, focusing on the last two words in the title. Can and will Americans take on the role of health citizens, with health care access as a civil right and full privacy protections, coupled with the responsibilities for self-care and health engagement, and the civic responsibility to vote and engage in civil discourse? We’ll round out this journey in tomorrow’s Health Populi. That’s the argument for health citizenship, our topic for tomorrow’s #5 of five posts plotlining HealthConsuming: From Health Consumer to Health Citizen, all this week in the Health Populi blog. The post The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 appeared first on HealthPopuli.com. The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 posted first on http://dentistfortworth.blogspot.com via Blogger The Promise of Digital Health and the Privacy Perils – HealthConsuming Explains, Part 4 What We Know We Know About ZIP Codes Food and Deaths of Despair HealthConsuming Explains Part 35/1/2019 “There’s a 15-year difference in the life expectancy between the richest and poorest Americans.” That’s the first sentence of Chapter 7 in my book, HealthConsuming: From Health Consumer to Health Citizen. This data point comes from research published in JAMA in April 2016 on the association between income and life expectancy in the U.S. (That’s endnote #399 in the back of the book, one of 519 notes I use to support the plotline).
Chapter 7 of my book, HealthConsuming: From Health Consumer to Health Citizen, is titled, “ZIP Codes, Genetic Codes, Food and Health.” The plot begins with the importance of “place,” our personal physical geographies and what they portend for our individual health — beyond our genetic code and inherited health risks. As the JAMA article notes, “The differences in life expectancy were correlated with health behaviors and local area characteristics.” This graphic on SDoH comes out of the book, illustrating the many external factors that influence personal and community health: among them, food, job security, education, environment (think: clean air if you live in Los Angeles, clean water if you live in Flint, Michigan), job and income security, and safe and green spaces among them. While not traditionally called out as a social determinant, I’ve added in broadband connectivity (with net neutrality baked in) as an influence on health and wellness, as well. To introduce the ideas in each chapter of the book, I ask big hairy “What If?” questions that I endeavor to answer. Here, I wonder, “What if… America reduced health disparities, increased health equity, and our ZIP codes didn’t determine our health outcomes and life expectancy?” The shocking reversal of life expectancy in the U.S. has been termed the “deaths of despair” by the brilliant researchers Anne Case and Sir Angus Deaton who are based at Princeton University. Their latest work on the phenomenon has revealed the role that (less) education plays as a risk factor for shorter lifespans, which I discuss in HealthConsuming as a tragic feature in U.S. public health — uniquely American versus the rest of the developed world. Opioids and social isolation (read the book Bowling Alone for more insights) contribute to this reversal-of-longevity.
“There is mounting evidence that some of these [SDoH] initiatives are associated with improved health outcomes and reduced health care utilization,” a report from Deloitte asserted in a new report on social determinants of health published this week. The growth of public sector incentives in Medicare for social supports, and growth of value-based payment in commercial plans, are forces nudging health care providers toward bundling SDoH services into targeted programs. The graphic from the Deloitte study illustrates a few of those strategies, including multi-tasking social needs, referring people to services with high-touch, partnering in the community with service providers, and monitoring and tweaking the SDoH interventions in a continuous-improvement mode. This seventh of eight chapters of HealthConsuming concludes: “Our communities are our local health ecosystems. Centuries’ worth of evidence, from Hippocrates in Athens, Greece to As U.S. policymakers are in the throes of designing an infrastructure bill allocating $trillions of taxpayer dollars, they should be mindful of “baking” social determinants of health into the plans. This concept is recommended in the last chapter of HealthConsuming as the plot moves to the question of whether health consumers will emerge as health citizens in America. Tomorrow, we’ll focus on the promise of digital health and the perils of privacy. Digital platforms and tools can help scale social determinants to people who need services. But without privacy protections that address our current reality of how we live and share online, the best-designed technology won’t be effective, or worse…could exacerbate already-challenged health outcomes and disparities. The post What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 appeared first on HealthPopuli.com. What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 posted first on http://dentistfortworth.blogspot.com via Blogger What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 What We Know We Know About ZIP Codes Food and Deaths of Despair HealthConsuming Explains Part 35/1/2019 “There’s a 15-year difference in the life expectancy between the richest and poorest Americans.” That’s the first sentence of Chapter 7 in my book, HealthConsuming: From Health Consumer to Health Citizen. This data point comes from research published in JAMA in April 2016 on the association between income and life expectancy in the U.S. (That’s endnote #399 in the back of the book, one of 519 notes I use to support the plotline).
Chapter 7 of my book, HealthConsuming: From Health Consumer to Health Citizen, is titled, “ZIP Codes, Genetic Codes, Food and Health.” The plot begins with the importance of “place,” our personal physical geographies and what they portend for our individual health — beyond our genetic code and inherited health risks. As the JAMA article notes, “The differences in life expectancy were correlated with health behaviors and local area characteristics.” This graphic on SDoH comes out of the book, illustrating the many external factors that influence personal and community health: among them, food, job security, education, environment (think: clean air if you live in Los Angeles, clean water if you live in Flint, Michigan), job and income security, and safe and green spaces among them. While not traditionally called out as a social determinant, I’ve added in broadband connectivity (with net neutrality baked in) as an influence on health and wellness, as well. To introduce the ideas in each chapter of the book, I ask big hairy “What If?” questions that I endeavor to answer. Here, I wonder, “What if… America reduced health disparities, increased health equity, and our ZIP codes didn’t determine our health outcomes and life expectancy?” The shocking reversal of life expectancy in the U.S. has been termed the “deaths of despair” by the brilliant researchers Anne Case and Sir Angus Deaton who are based at Princeton University. Their latest work on the phenomenon has revealed the role that (less) education plays as a risk factor for shorter lifespans, which I discuss in HealthConsuming as a tragic feature in U.S. public health — uniquely American versus the rest of the developed world. Opioids and social isolation (read the book Bowling Alone for more insights) contribute to this reversal-of-longevity.
“There is mounting evidence that some of these [SDoH] initiatives are associated with improved health outcomes and reduced health care utilization,” a report from Deloitte asserted in a new report on social determinants of health published this week. The growth of public sector incentives in Medicare for social supports, and growth of value-based payment in commercial plans, are forces nudging health care providers toward bundling SDoH services into targeted programs. The graphic from the Deloitte study illustrates a few of those strategies, including multi-tasking social needs, referring people to services with high-touch, partnering in the community with service providers, and monitoring and tweaking the SDoH interventions in a continuous-improvement mode. This seventh of eight chapters of HealthConsuming concludes: “Our communities are our local health ecosystems. Centuries’ worth of evidence, from Hippocrates in Athens, Greece to As U.S. policymakers are in the throes of designing an infrastructure bill allocating $trillions of taxpayer dollars, they should be mindful of “baking” social determinants of health into the plans. This concept is recommended in the last chapter of HealthConsuming as the plot moves to the question of whether health consumers will emerge as health citizens in America. Tomorrow, we’ll focus on the promise of digital health and the perils of privacy. Digital platforms and tools can help scale social determinants to people who need services. But without privacy protections that address our current reality of how we live and share online, the best-designed technology won’t be effective, or worse…could exacerbate already-challenged health outcomes and disparities. The post What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 appeared first on HealthPopuli.com. What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 posted first on http://dentistfortworth.blogspot.com via Blogger What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 What We Know We Know About ZIP Codes Food and Deaths of Despair HealthConsuming Explains Part 35/1/2019 “There’s a 15-year difference in the life expectancy between the richest and poorest Americans.” That’s the first sentence of Chapter 7 in my book, HealthConsuming: From Health Consumer to Health Citizen. This data point comes from research published in JAMA in April 2016 on the association between income and life expectancy in the U.S. (That’s endnote #399 in the back of the book, one of 519 notes I use to support the plotline).
Chapter 7 of my book, HealthConsuming: From Health Consumer to Health Citizen, is titled, “ZIP Codes, Genetic Codes, Food and Health.” The plot begins with the importance of “place,” our personal physical geographies and what they portend for our individual health — beyond our genetic code and inherited health risks. As the JAMA article notes, “The differences in life expectancy were correlated with health behaviors and local area characteristics.” This graphic on SDoH comes out of the book, illustrating the many external factors that influence personal and community health: among them, food, job security, education, environment (think: clean air if you live in Los Angeles, clean water if you live in Flint, Michigan), job and income security, and safe and green spaces among them. While not traditionally called out as a social determinant, I’ve added in broadband connectivity (with net neutrality baked in) as an influence on health and wellness, as well. To introduce the ideas in each chapter of the book, I ask big hairy “What If?” questions that I endeavor to answer. Here, I wonder, “What if… America reduced health disparities, increased health equity, and our ZIP codes didn’t determine our health outcomes and life expectancy?” The shocking reversal of life expectancy in the U.S. has been termed the “deaths of despair” by the brilliant researchers Anne Case and Sir Angus Deaton who are based at Princeton University. Their latest work on the phenomenon has revealed the role that (less) education plays as a risk factor for shorter lifespans, which I discuss in HealthConsuming as a tragic feature in U.S. public health — uniquely American versus the rest of the developed world. Opioids and social isolation (read the book Bowling Alone for more insights) contribute to this reversal-of-longevity.
“There is mounting evidence that some of these [SDoH] initiatives are associated with improved health outcomes and reduced health care utilization,” a report from Deloitte asserted in a new report on social determinants of health published this week. The growth of public sector incentives in Medicare for social supports, and growth of value-based payment in commercial plans, are forces nudging health care providers toward bundling SDoH services into targeted programs. The graphic from the Deloitte study illustrates a few of those strategies, including multi-tasking social needs, referring people to services with high-touch, partnering in the community with service providers, and monitoring and tweaking the SDoH interventions in a continuous-improvement mode. This seventh of eight chapters of HealthConsuming concludes: “Our communities are our local health ecosystems. Centuries’ worth of evidence, from Hippocrates in Athens, Greece to As U.S. policymakers are in the throes of designing an infrastructure bill allocating $trillions of taxpayer dollars, they should be mindful of “baking” social determinants of health into the plans. This concept is recommended in the last chapter of HealthConsuming as the plot moves to the question of whether health consumers will emerge as health citizens in America. Tomorrow, we’ll focus on the promise of digital health and the perils of privacy. Digital platforms and tools can help scale social determinants to people who need services. But without privacy protections that address our current reality of how we live and share online, the best-designed technology won’t be effective, or worse…could exacerbate already-challenged health outcomes and disparities. The post What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 appeared first on HealthPopuli.com. What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3 posted first on http://dentistfortworth.blogspot.com via Blogger What We Know We Know About ZIP Codes, Food, and Deaths of Despair – HealthConsuming Explains, Part 3
Consumers know what good retail looks and feels like, and are focusing that experiential lens on health care, Aflac found when their Workforces Survey polled Americans on what they’d like their health insurance shopping process to feel like. One in two people said, “like Amazon,” and another 20% of folks said, “like retail.” Chapter 3 of HealthConsuming is titled, “How Amazon Has Primed Health Consumers,” and explains this re-shaping of patient expectations. Here’s one of my paragraphs from the chapter, noting that, “Health consumers are hungry for Amazon’s brand of transparency, convenience, and streamlined interactions for medical care. The Amazon Prime-ing of the U.S. consumer has raised peoples’ expectations of what health care services could be: personalized, customized, anticipatory, immediate or on-schedule, and convenient – where we live, work, play, pray, learn and even drive.”
In the past couple of months, Amazon announced many health-related plans and developments, including:
For health consumers, Amazon’s multi-tasking efforts are re-shaping health care service delivery and channeling. Most importantly, in this immediate moment, Amazon has re-shaped patients as health consumers — our expectations for what is possible in health care delivery, price transparency, peer-to-peer advice, and convenience. In tomorrow’s Health Populi, we’ll dive into a third key theme in HealthConsuming: that’s what we know-we-know about ZIP codes, food, deaths of despair, and the social determinants of health. Where we live portends how healthy we are…and why spending on social care is key to addressing health and longer life spans…the personal health version of surviving a death star. On Thursday, my post will raise Amazon’s role in health/care again, looking more deeply into the promise of digital health and the perils of privacy for health, retail, and other personal data. Amazon isn’t just about convenient delivery of health care “things.” It’s about the data generated by those transactions, which help to construct profiles on you and me. Using such profiles can be very helpful for health, if that’s the intent of the data-miner. But as the Financial Times pointed out today in an op-ed written by its editorial board, “Platform companies from Amazon to Google to Apple are getting deep into the healthcare field, allowing us to do everything from communicate with doctors to check on prescriptions. The privacy implications are troubling….they are [also] surveilling consumers at the same time — gathering, analysing and, in many cases, selling sensitive data. In many countries, personal healthcare data are subject to strict regulation. In the US, the Health Insurance Portability and Accountability Act (HIPAA) imposes criminal and civil penalties for breaching confidentiality of healthcare data. But the rules apply only to entities covered by HIPAA such as healthcare plans and providers, or clearing houses that process healthcare claims.” Stay tuned to tomorrow’s post, on social determinants of health and social spending. By Friday, the dots will converge on the topic of morphing from health consumers to health citizens. The post Health Consumers Are Now Amazon-Primed for Healthcare – HealthConsuming Explains, Part 2 appeared first on HealthPopuli.com. Health Consumers Are Now Amazon-Primed for Healthcare – HealthConsuming Explains, Part 2 posted first on http://dentistfortworth.blogspot.com via Blogger Health Consumers Are Now Amazon-Primed for Healthcare – HealthConsuming Explains, Part 2 |
ABOUT US
I am a certified Dietitian and won many accolades for my award winning The Nutrition Guide. I am also co-founder of Step Consulting and guiding you to live a healthier you for more than 20 years. My Other Profiles: |
 Today, we can also call on Alexa to remind us to take medications, play nostalgic music when we are lonely, check our physical activity status with Fitbit, and query WebMD about a symptom. Just last month, Amazon announced HIPAA-compliant privacy bundled into Alexa skills with Atrium Health, Boston Children’s Hospital, CIGNA, ExpressScripts, Livongo, and Swedish Health Connect.
Today, we can also call on Alexa to remind us to take medications, play nostalgic music when we are lonely, check our physical activity status with Fitbit, and query WebMD about a symptom. Just last month, Amazon announced HIPAA-compliant privacy bundled into Alexa skills with Atrium Health, Boston Children’s Hospital, CIGNA, ExpressScripts, Livongo, and Swedish Health Connect. Today, the Brookings Institution convened a meeting on
Today, the Brookings Institution convened a meeting on 
 As patients now assume the role of health consumer, they rationally expect retail-level experiences with greater first-dollar payment for health insurance, health care services and medical products like prescription drugs.
As patients now assume the role of health consumer, they rationally expect retail-level experiences with greater first-dollar payment for health insurance, health care services and medical products like prescription drugs.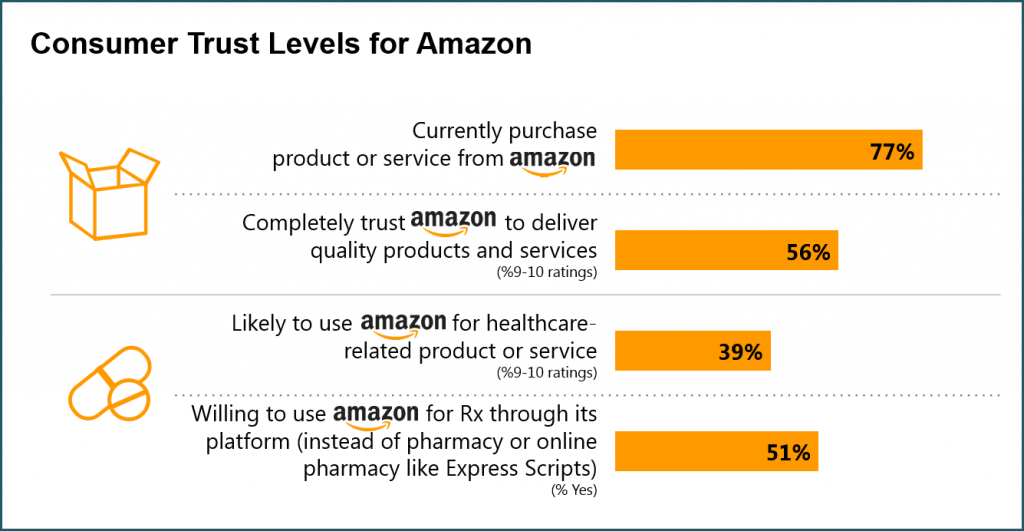 People trust Amazon for daily retail experiences. The bar chart from research by Market Strategies shows that a plurality of consumers also trusts Amazon to try on for healthcare products and services. The company has been multi-tasking a broad range of tactics throughout the health care ecosystem. Every publicly traded market segment Amazon has touched has had moments of shattering stock prices.
People trust Amazon for daily retail experiences. The bar chart from research by Market Strategies shows that a plurality of consumers also trusts Amazon to try on for healthcare products and services. The company has been multi-tasking a broad range of tactics throughout the health care ecosystem. Every publicly traded market segment Amazon has touched has had moments of shattering stock prices. Jim Cramer of CNBC’s Mad Money has been studying up on digital health, recently recommending that Apple buy Epic, the health IT behemoth. (See more on that recommendation, and subsequent social media frenzy,
Jim Cramer of CNBC’s Mad Money has been studying up on digital health, recently recommending that Apple buy Epic, the health IT behemoth. (See more on that recommendation, and subsequent social media frenzy,  RSS Feed
RSS Feed
